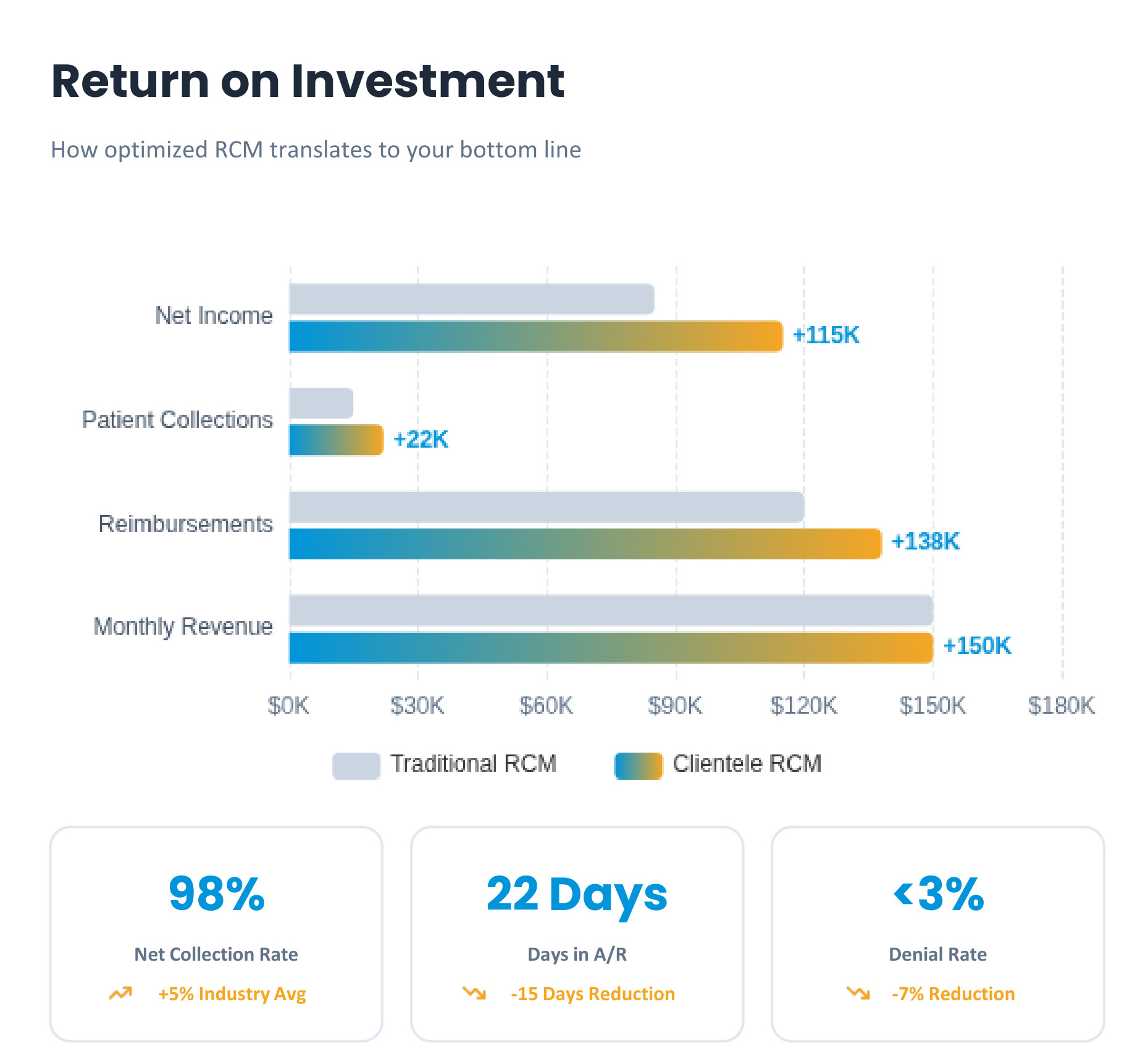
Revenue Cycle Management Case Studies
- The Challenge
A mid-sized multi-specialty group faced severe cash flow issues due to a backlog of unpaid claims.
Documentation delays and poor coding quality led to a surge in denials.
- High denial rate due to coding errors
- Provider documentation lag > 7 days
120+
DAYS IN A/R
- The Action
- implemented 24h turnaround requirement for charts.
- AI pre-coding with Human-in-the-Loop verification.
- Corrected claims before submission to payers.
- The Result
Clientele RCM deployed a rapid response team to overhaul the documentation workflow and implement stringent quality checks.

Case Study: Personal Injury Claims
- The Challenge
An injury claims for provider experienced zero payments on high-value claims because they were incorrectly routed to commercial health insurance instead of Auto/Workers’ Compensation.
- Immediate denials from Commercial Payers
- Failure to bill liable third-party carriers
ZERO
REVENUE ON MISROUTED CLAIMS
- The Action
Clientele RCM implemented a specialized front-end intake process to identify accident details and route claims to the correct liable payer immediately.
- Auto-detection of injury codes to trigger Auto/WC workflows.
- Ensuring accident dates and claim numbers are captured.
- Re-billed past denials to correct carriers.
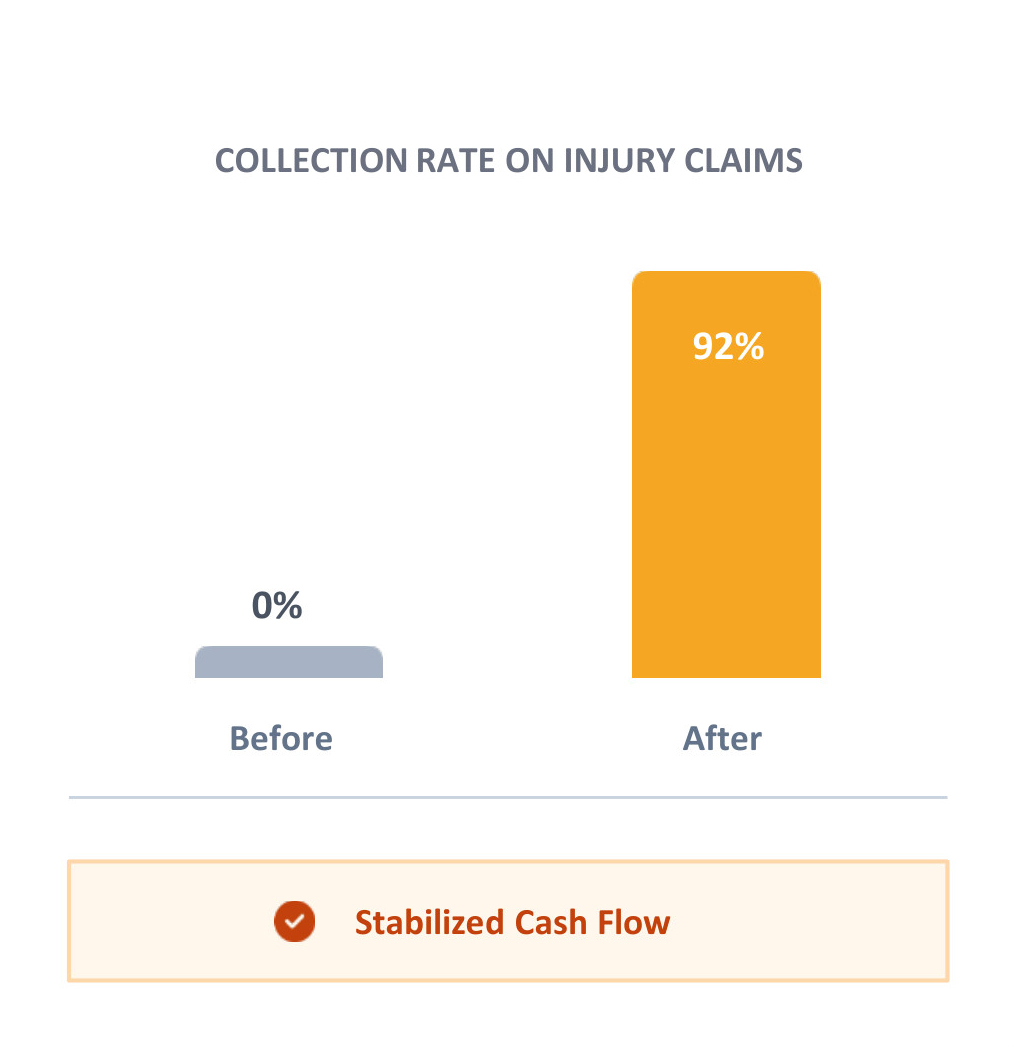
- The Result
The facility successfully recovered payments from correct carriers and stabilized cash flow by stopping the denial cycle at the source.
Case Study: Clearinghouse Resolution
A high-volume practice experienced significant revenue loss due to “Timely Filing Limit” (TFL) denials. Claims appeared sent but were never acknowledged by the payer.
The Challenge
Trapped Denials
Claims were getting stuck at the clearinghouse layer without rejection notices reaching the practice until after the filing deadline passed.
- No payer acknowledgement received
- False "Submitted" status in PM system
- Rising write-offs due to TFL
The Action
Audit & Tracking
We conducted a comprehensive audit of payer enrollment IDs and implemented a “beyond the gateway” tracking protocol.
- Audited EDI enrollment & Payer IDs
- Configured 277CA acknowledgement parsing
- Manual audit of "At Clearinghouse" buckets
The Result
Restored Throughput
Complete elimination of avoidable TFL denials and restoration of clean claim throughput with 100% status visibility.
100%
CLAIM VISIBILITY RESTORED
- TFL Denials Eliminated
Case Study: Out-of-Network Optimization
- The Challenge
The practice was suffering from significant revenue leakage due to incorrect assumptions about Out-of-Network (OON) coverage, leading to automatic write-offs rather than pursuit of payment.
- Excessive write-offs based on OON status
- Lack of distinction between no-coverage and OON
High %
REVENUE WRITE-OFFS
- The Action
Clientele RCM implemented a granular segmentation strategy to differentiate between genuine lack of benefits and OON reimbursement opportunities.
- Separated provider OON status from patient benefit gaps.
- Applied specific follow-up logic for OON claims.
- Pursued OON benefits instead of writing off.
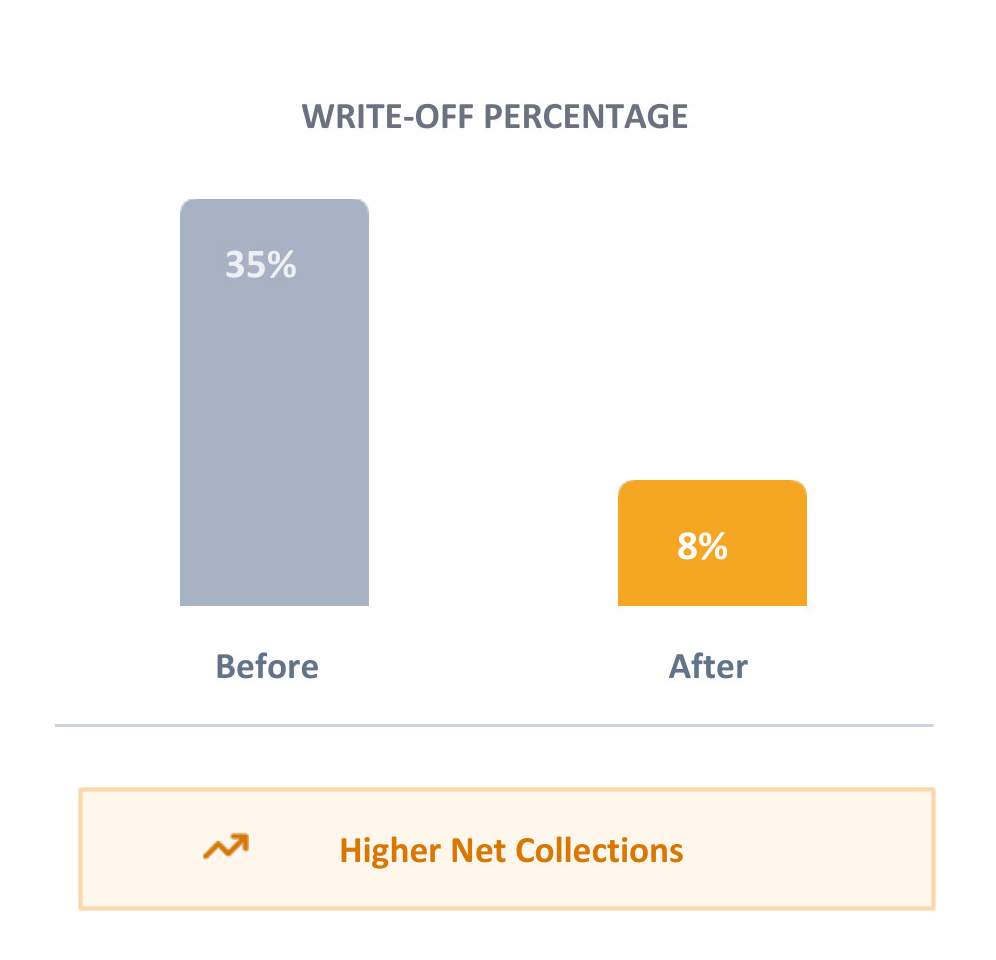
- The Result
By correctly identifying and pursuing collectible OON claims, the practice drastically reduced unnecessary write-offs and increased net collections.
Case Study: Negotiation Success
- The Challenge
The provider faced significant revenue leakage on Out-of-Network (OON) claims, with commercial payers consistently underpaying or repricing claims to near-Medicare rates.
- Low reimbursement on high-value claims
- Lack of negotiation leverage with payers
Low %
REIMBURSEMENT RATE
- The Action
Clientele RCM implemented a dedicated negotiation team to engage third-party payers, backed by robust clinical documentation to substantiate charges.
- Direct engagement with payer settlement teams.
- Leveraging state laws and medical necessity.
- Proof of complexity to justify higher rates.
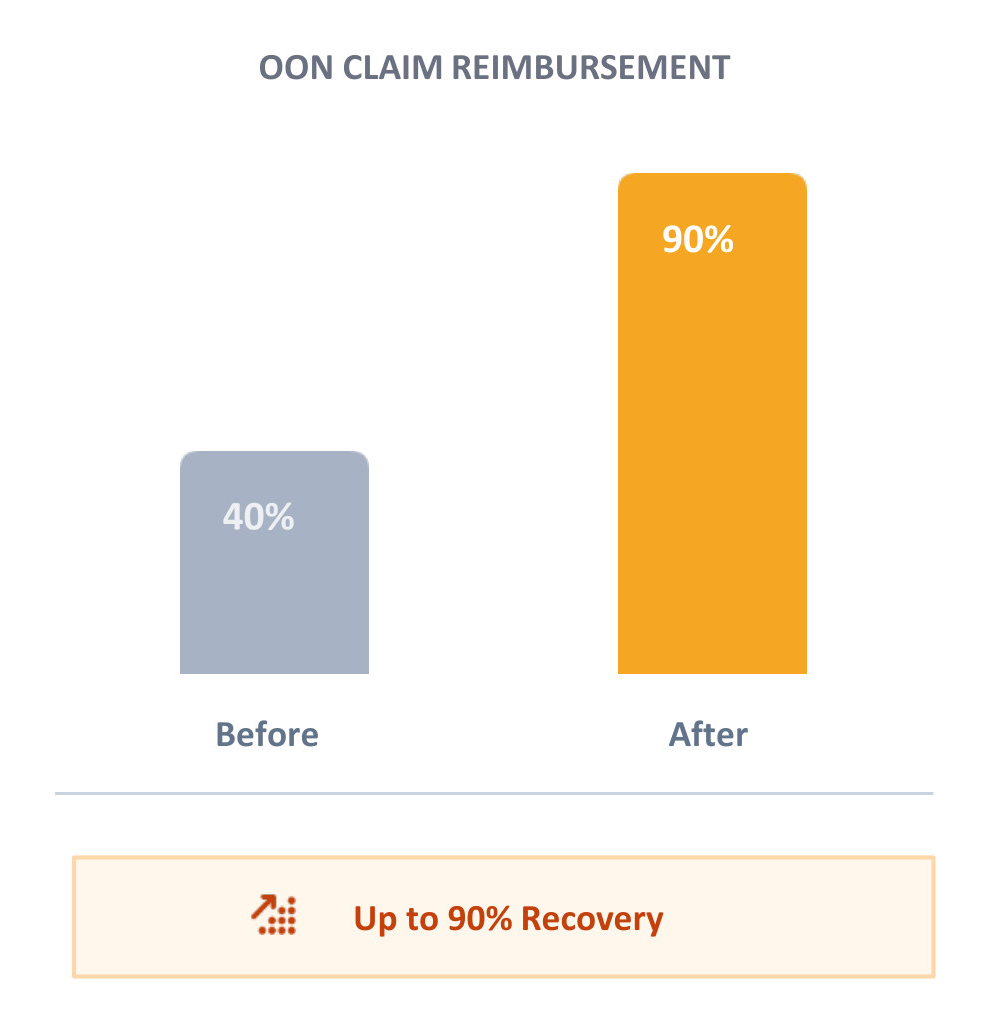
- The Result
The strategy yielded a dramatic increase in payment recovery, securing favorable settlements on previously underpaid claims.
Financial Model & ROI
- Zero-Risk Onboarding Model
We believe in proving our value before you pay. Experience our premium RCM services with absolutely no financial risk during the transition.The provider faced significant revenue leakage on Out-of-Network (OON) claims, with commercial payers consistently underpaying or repricing claims to near-Medicare rates.
- First 2 Months of Billing at NO COST
- Zero Implementation Fees
- No Long-Term Lock-in During Pilot
- Engagement Model
Transparent percentage-of-collections pricing model ensures our goals are perfectly aligned. We only get paid when you get paid.